

A. K. Azad1*, Wan Azizi WS1,2, Adham SA2, Yee BL2
1Department of Basic Medical Sciences, Kulliyyah of Pharmacy, International Islamic University Malaysia, Kuantan, Pahang, Malaysia.
2Natural Medicinal Product Center, Kulliyyah of Pharmacy, International Islamic
University Malaysia, Kuantan, Pahang, Malaysia.
Corresponding Author:
Asst. Prof. Dr. Wan Mohd Azizi Wan Sulaiman,
Department of Basic Medical Sciences,
Faculty of Pharmacy, International Islamic University Malaysia,
Jalan Sultan Ahmad Shah, 25200 Kuantan, Pahang, Malaysia.
Tel: 5704871, Fax: 5706775, Mobile No: 060179363729,
Abstract
Objective:This study aimed to evaluate the benefit of Maggot Debridement Therapy (MDT) in the treatment of diabetic foot ulcer (DFU) patient. Materials and methods: This study records result in diabetic foot wounds treated with larva debridement versus those treated by traditional debridement alone. In this arrangement of 42 patients treated with MDT. Results: There was no critical contrast in result among the gatherings. Conclusion: This study can be concluded that MDT as powerful as traditional debridement in the treatment of diabetic foot ulcers. It would be an achievable different option for diabetic foot ulcer treatment.
Keywords: Wound, larva, debridement, foot-ulcer
Introduction
Natural phytochemicals have been reported to possess a wide range of biological activities including antioxidant, antimicrobial and anti-inflamatory properties (Azad et al., 2012; Azad et al., 2013).Maggot debridement therapy (MDT) is a therapeutic use of sterile larvae of Lucilia Cuprina from the entomology lab of IMR to treat non healing diabetic foot ulcers. In Malaysia, MDT has been approved by MOH as one of the standard treatment for wound management. It has been used widely in both government and private hospitals (Paul et al., 2009).
Chronic wounds, such as pressure sores and diabetic or vascular ulcers, are associated with high morbidity and, to a lesser extent, mortality (Beasley and Hirst, 2004). Chronic wounds are notoriously difficult to treat because they usually take the form of non-healing ulcers with fibrotic tissue, dead necrotic slough, and multiple infections (Gupta, 2008). An important issue in wound management is the process called debridement (Dumville et al., 2009) which is defined as the removal of foreign debris and devitalized or contaminated tissues from a wound bed so that the surrounding healthy tissues are exposed. Clinicians may debride wounds using various methods, including surgery, conservative sharp, high-pressure fluid irrigation, ultrasonic mist, autolysis, or enzymatic agents (Gray, 2008). .
One of the ‘old’ techniques in wound care is maggot debridement therapy (MDT). MDT is also known as maggot therapy, biodebridement, or larval therapy. In this therapy live fly larvae are applied to the patient's wounds to achieve debridement, disinfection and resulted ultimately wound healing. MDT is aplicable for open wounds and ulcers that contain necrotic tissues with or without infection (Sherman, 2009).
MDT uses freshly sterile larvae of the common green-bottle fly, Phaenicia sericata, which is also an artificially induced myiasis raised under controlled clinical conditions. This type of therapy has several beneficial effects on wounds and ulcers also including debridement, disinfection and increased wound healing (Veen, 2008). The beneficial effects of using larvae were first noted in 1557 (Nigam et al., 2006) but with the introduction and widespread use of antibiotics in the 1940s, it was gradually neglected by doctors. In recent years, with the rising incidence of drug resistance (Azad et al., 2012), there has been renewed interest in using maggots in chronic wound management, particularly in treating wounds infected with methicillin resistant Staphylococcus aureus (MRSA) and other drug-resistant pathogens (Goldstein, 1931 and Mumcuoglu, 2001).Current evidence supporting MDT for chronically infected lesions comes from several small clinical trials.
Materials and methods
Study Design: A single subject study design which involves a pre-test followed by an intervention, and a post-test, in order to determine the effect of MDT on patients with DFU, in one particular patient at a time.
Setting: Maggot Debridement Therapy Center in Kuala Lumpur and Kuantan, collaboration of International Islamic University Malaysia and Medical BioTherapy Sdn Bhd (Bionexus company under Malaysian Biotechcorp).
Patient Selection: The study was carried out on eleven (42) patients.
Inclusion criteria: Patient aged 30-70 years. Diabetic foot ulcer with slough, estimated medium wound size of 3cm x 11cm, required re-debridement, indicated of sepsis as antibiotics were given, patient's willingness to try natural medicinal products (maggots).
Exclusion criteria: The wound with profusely bleeding, medium wound size with deep “tracking”, ischemic wound, gangrenous wound, patients who have entomophobia, patients who refused to try natural medicinal products.
Data Analysis (Wound Progress): This case study is based on case controlled where patient serve as control involving pre and post test. All the patients were taken photograph before starting the MDT and each time of treatment. Wound assessment was done by visual grading based on wound outcome scoring system by Aaron, Paul et al. 2009.
Table 1. Outcome classification of MDT
|
Grade |
Sub-grade |
Outcome |
|
Healed |
1A |
Suitable for SSG, flap coverage or self-healing |
|
|
1B |
Debridement + SSG/ flap coverage |
|
|
1C |
Assisted debridement in between to remove necrotic tendons or exposed bone |
|
Unhealed |
2 |
Surgical debridement (MDT abandoned) |
|
|
3A |
Minor amputation (below ankle) |
|
|
3B |
Major amputation (above ankle) |
|
Others |
4 |
Others (patient withdrawal, discontinuation, death, etc.) |
Table 2. Data shown the expected results after treatment with maggots
|
Patient |
Wound Size Estimate |
Amount of maggots per treatment |
Duration of Treatment (from starting till ending) in Days |
Classification for MDT |
|
P1 |
4 cm×7 cm |
50,50,50,100 |
32 |
Healed- 1C; assisted debridement + 2 rays amputation |
|
P2 |
6 cm×9 cm |
100,100,100, 150 |
20 |
Others- 4; discontinuation due to other systemic disorder |
|
P3 |
5 cm×8 cm |
50,50,100 |
43 |
Healed- 1A; wound clean, for self healing |
|
P4 |
5 cm×7 cm |
100,100 |
51 |
Healed- 1C; assisted debridement in between to remove necrotic tendons or exposed bones |
|
P5 |
3 cm×6 cm |
50,50,200 |
28 |
Healed- 1A; wound clean, for self healing |
|
P6 |
3 cm×6 cm |
300,300 |
50 |
Healed- 1A; wound clean, for self healing |
|
P7 |
5 cm×10 cm |
1000 |
13 |
Healed- 1A; wound clean, for self healing |
|
P8 |
3 cm × 8 cm |
200 |
11 |
Healed- 1A; wound clean, for self healing |
|
P9 |
5 cm×10 cm |
400,200,400, 400 |
22 |
Healed- 1A; wound clean, for self healing |
|
P10 |
4 cm×5 cm |
300,200,200 |
31 |
Healed- 1A; wound clean, for self healing |
|
P11 |
6 cm×11 cm |
350,400,200, 100 |
32 |
Healed- 1A; wound clean, for self healing |
Results and Discussions
The role of MDT in treating diabetic foot ulcers has been demonstrated clearly by the improvement of and speeding up the wound healing process. The debridement and antiseptic properties of MDT helps to clear and clean the debris and necrotic tissues. In addition to that, it also promotes granulation tissues and nerve stimulations.
MDT has also managed to reduce the cost of wound management by shortens the length of hospitalization stay and avoidance of operation and amputation procedures.
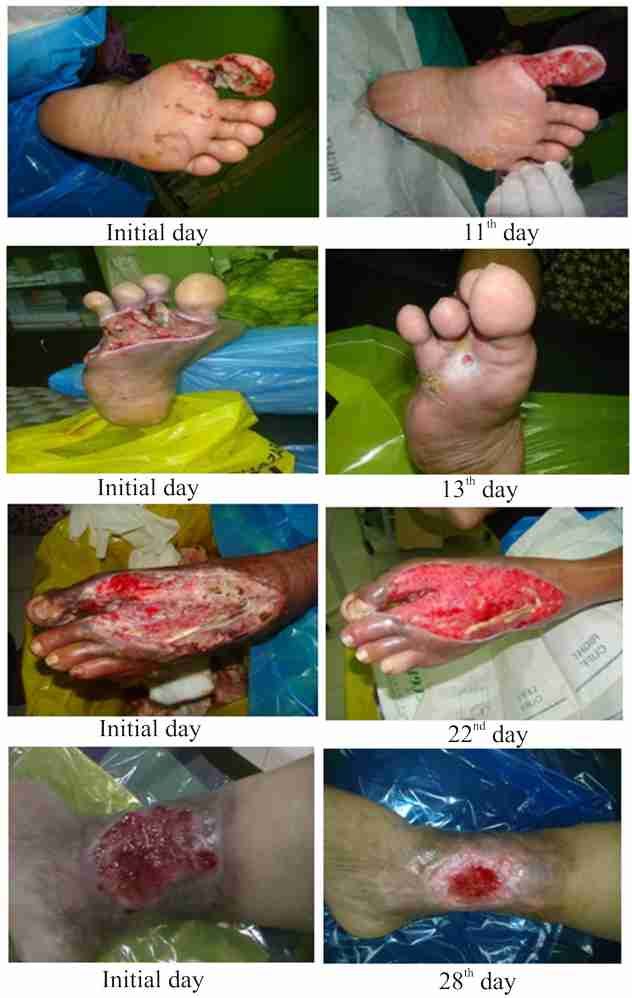
Figure 1. Observation results after treatment with maggots
Our patient’s entire wound completely healed after an average of three times maggot treatment, with average vial of 200 (Figure 1). The average time for the wound condition free from slough was 30 days. Subsequently, patients will continue the normal dressing and skin graft procedures. These data’s supported our findings of shorter duration of healing and cost saving as they have been followed up as an outpatient.
Conclusion
This study indicates the beneficial effect of MDT towards diabetic foot ulcer patient in our Maggot Treatment centers. However, we propose a proper and large scale studies to further confirm our findings.
Acknowledgement
This study was supported by the Natural Product Research Center, Faculty of Pharmacy, International Islamic University of Malaysia.
Conflict of interest
All authors have no conflict of interest.
References
Azad AK, Awang M, Rahman MM, Akter SF. 2012. Biological and pre-clinical trial evaluation of a local medicinal plant Bacopa monnieri (L.) Penn. International Journal of Current Research and Review, 4(19): 92-99.
Azad AK, Wan Azizi WS, Babar ZM, Labu ZK, Zabin S. 2013. An Overview on Phytochemical, Anti-Inflammatory and.Anti-Bacterial Activity of Basella alba Leaves Extract. Middle East Journal of Scientific Research, 14 (5): 650-655.
Azad MAK, Ansary MRH, Akter MA, AlMamun SMM, Uddin M, Rahman MM. Disposal Practice for Unused Medications among the Students of the International Islamic University Malaysia. Journal of Applied Pharmaceutical Science, 02(07): 101-106.
Beasley WD, Hirst G. Making a meal of MRSA-the role of biosurgery in hospital-acquired infection. Journal of Hospital Infection, 56: 6–9.
Dumville JC, Worthy G, Bland JM, Cullum N, Dowson C, Iglesias C, et al.2009. Larval therapy for leg ulcers (VenUS II): randomised controlled trial. British Medical Journal, 338: 773.
Goldstein HI. 1931. Maggots in the treatment of wound and bone infections. AmericanJournal of Bone Joint Surgery, 13: 476–478.
Gray M. 2008. Is larval (maggot) debridement effective for removal of necrotic tissue from chronic wounds? Journal of Wound Ostomy and Continence Nursing, 35(4): 378-384.
Gupta A. 2008. A review of the use of maggots in wound therapy. Annal Plastic Surgery, 60: 224–227.
Mumcuoglu KY. 2001.Clinical applications for maggots in wound care. American Journal of Clininical Dermatology, 2: 219–227.
Nigam Y, Bexfield A, Thomas S, Ratcliffe NA. 2006. Maggot therapy: the science and implication for CAM part II—maggots combat infection. Evidence Based Complementary Alternative Medicine, 3: 303–308.
Paul AG, Ahmad NW, Lee HL, Ariff AM, Saranum M, Naicker AS, Osman Z. 2009. Maggot debridement therapy with Luciliacuprina: a comparison with conventional debridement in diabetic foot ulcers. International Wound Journal, 6(1): 39-46.
Sherman RA. 2009. Maggot therapy takes us back to the future of wound care: new and improved maggot therapy for the 21st century. Journal of Diabetes Science and Technology, 3 (2):336–344.
Van Veen LJ. 2008. Maggot debridement therapy: a case study. Journal of Wound Ostomyand Continence Nursing, 35: 432–436.